
| Volume 16 – Number 2 | Summer 1999 |
TABLE OF CONTENTS
 |
COMMON ABBREVIATIONS
BMI: body mass index (kg/m2)
CAD: coronary artery disease
CHD: coronary heart disease
CHO: carbohydrate
CI: confidence interval
CVD: cardiovascular disease
ene: energy
HDL: high density lipoprotein
LDL: low density lipoprotein
Lp(a): lipoprotein (a)
MI: myocardial infarction
MUFA: monounsaturated fatty acids
NCEP: National Cholesterol Education Program
P:S: dietary polyunsaturated:saturated fat ratio
PUFA: polyunsaturated fatty acids
RR: relative risk
SFA: saturated fatty acids
TAG: triacylglycerol
VLDL: very low density lipoprotein
Egg Consumption Not Associated with CVD and Stroke
For decades, eggs represented the visual icon for dietary cholesterol for many health conscious consumers and became a food to limit in the pursuit of heart health. But according to 2 large prospective epidemiological surveys, the Nurses’ Health Study (NHS) and the Health Professionals Follow-up Study (HPFS), it’s not eggs that increase CVD risk but rather the high saturated fat company eggs keep on the plate. Data from the NHS evaluated the 14 year (1980-1994) eating habits of 80,082 healthy women, while the HPFS measured the 8 year (1986-1994) eating habits of 37,851 males. Males in the HPFS were dentists, optometrist, pharmacists, podiatrists, and veterinarians, between the ages of 40 to 75 years at the start of the study. Nurses in the NHS were 34 to 59 years old at baseline. All study subjects were initially free of CVD, hypercholesterolemia, diabetes, and cancer at study onset. Biennial questionnaires were used to screen for the occurrence of fatal CHD, nonfatal MI and strokes, and reported cases were confirmed. During the follow-up period, 866 cases of CHD and 258 cases of stroke were confirmed in men and 939 cases of CHD and 563 cases of stroke were confirmed in women.
Based on food frequency questionnaires, high egg consumption was associated with many negative lifestyle and dietary habits in male health professionals. They were more likely to smoke; exercise less; consume more saturated fats in the form of red meat, bacon, whole milk; and eat less fruits and vegetables. The total grams of saturated fat intake increased directly with number of egg consumed. These trends, except for bacon intake, were less evident in nurses. During the study period, the average per capita egg consumption decreased from 2.3 egg/week in 1986 to 1.6 egg/week in 1990 in males and 2.8 egg/week in 1980 to 1.4 egg/week in 1990 in females. Also, eggs typically replaced breakfast cereals intake. The accuracy of food frequency questionnaires was confirmed by validation studies.
Using data from NHS and HPFS, Hu et al. tested the hypothesis that there is a direct relationship between egg intake and CHD risk and stroke. The investigators found that consumption of up to 1 egg per day had no overall impact on the risk of CVD among healthy men and women. For example, initially, the male cohorts with the highest egg intakes (> 1 egg/day) were only slightly more likely to develop CHD than males who 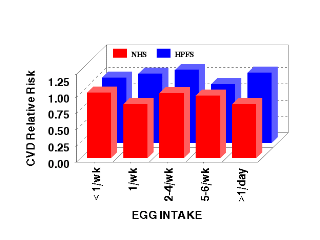 ate less than 1 egg/week. However, when smoking, dietary fiber intake, and other risk factors for CHD were included in the analysis, this association was null. In women, there was no relationship between CHD and egg intake at any level. The adjustment for cohorts’ bacon intake further attenuated the association between egg intake and CHD. The adjusted relative risk for CHD was 1.0 for 1 egg/week, 1.04 for 2-4 eggs/week, 0.78 for 5-6 eggs/week, and 0.93 for 1 egg/day in males and 0.81, 0.96, 0.91, and 0.78, respectively in females. Based on a small number of subjects who ate more than 2 eggs per day, the multivariate RR for CHD was 0.76 in women and 1.10 in men. Further analysis suggested that neither short-term nor long-term egg consumption was associated with CHD risk. As in the case of CHD risk, egg consumption was not associated with increased total stroke, ischemic stroke, or hemorrhagic stroke.
ate less than 1 egg/week. However, when smoking, dietary fiber intake, and other risk factors for CHD were included in the analysis, this association was null. In women, there was no relationship between CHD and egg intake at any level. The adjustment for cohorts’ bacon intake further attenuated the association between egg intake and CHD. The adjusted relative risk for CHD was 1.0 for 1 egg/week, 1.04 for 2-4 eggs/week, 0.78 for 5-6 eggs/week, and 0.93 for 1 egg/day in males and 0.81, 0.96, 0.91, and 0.78, respectively in females. Based on a small number of subjects who ate more than 2 eggs per day, the multivariate RR for CHD was 0.76 in women and 1.10 in men. Further analysis suggested that neither short-term nor long-term egg consumption was associated with CHD risk. As in the case of CHD risk, egg consumption was not associated with increased total stroke, ischemic stroke, or hemorrhagic stroke.
When subjects with other risk factors for CHD were included in the analysis, only diabetics were found to have increased CHD risk associated with high egg intake. The multivariate relative risk for 1 egg/week was 1.0 and 1.0, 1 egg/week 1.0 and 0.91, 2-4 egg/week 1.16 and 1.05, 5-6 eggs/week 1.16 and 1.87, and 1 egg/day 2.02 and 1.49 for diabetic men and women, respectively. Results from these large epidemiological studies clearly show that it possible to eat an egg a day without increasing CHD risk in healthy men and women. This in part may relate to the fact that eggs contain antioxidants, folate, and other B vitamins which have been shown to reduce CHD risk. And by substituting for breakfast cereals, egg consumption can both increase HDL cholesterol and decrease TAG levels. The relationship between egg consumption and CVD seen with diabetics might have been “related to abnormal cholesterol transport due to decreased levels of apolipoprotein E and increased levels of apolipoprotein C-III” and thus needs further studies to evaluate the situation.
Hu FB, Stampfer MJ, Rimm EB, et al. A prospective study of egg consumption and risk of cardiovascular disease in men and women. JAMA. 1999;281-1387-1394.
Key Messages
- Egg consumption is not associated with CHD risk in healthy men and women.
- Antioxidants, folate, other B vitamins, and unsaturated fats found in eggs can potentially counterbalance small effects of cholesterol in eggs on plasma LDL levels.
- Egg consumption is associated with improved plasma HDL and TAG levels.
- The total grams of saturated fat intake increased directly with number of egg consumed.
- Higher egg consumption is associated with increased CHD risk in people with diabetes.
|
Editor’s Comment It would be easy to dismiss the findings of the Nurses’ Health Study and the Health Professionals Follow-Up Study as just a single report with an unexpected finding. The fact is the findings reported by Hu and colleagues are not in the least unexpected or an aberrant, one-of-a-kind report. Over the past five years there have been numerous reports of a null relationship between cholesterol intakes, plasma cholesterol levels and CVD incidence. Data from MRFIT indicated that neither total dietary cholesterol nor egg consumption were related to the plasma cholesterol levels of 12,553 men (1). Results from the Framingham Heart Study indicated no relationship between dietary cholesterol and either plasma cholesterol levels or heart disease incidence in 1,422 women (2). Data from both the Nurses’ Health Study of 80,082 women (3) and the Health Professionals Follow-Up Study of 43,757 men (4) indicated that dietary cholesterol was not significantly related to CHD morbidity or mortality. Analysis of data from the Lipid Research Clinics Follow-Up Study in 4,546 men and women (5) found no relationship between dietary cholesterol and CHD incidence. The Alpha-Tocopherol, Beta-Carotene Cancer Prevention Trial in 21,930 men (6) also reported that dietary cholesterol was not significantly related to CHD incidence. The fact is that over the last five years I know of no report from any large epidemiological trial indicating a positive relationship between dietary cholesterol and heart disease risk. Rather than questioning the validity of the observations reported by Hu et al.(7) maybe it is time that the nutritional scientists question the validity of those thirty year old studies which suggested that dietary cholesterol was a factor in CVD incidence. 1. Tillotson JL, Bartsch GE, Gorder D, Grandits GA, Stamler J. Food group and nutrient intakes at baseline in the Multiple Risk Factor Intervention Trial. Am J Clin Nutr 1997;65 (Suppl):228S-257S. 2. Millen BE, Franz MM, Quatromoni PA, et al. Diet and plasma lipids in women .1. Macronutrients and plasma total and low-density lipoprotein cholesterol in women: The Framingham nutrition studies. J Clin Epidemiol 1996;49:657-663. 3. Hu FB, Stampfer MJ, Manson JE, et al. Dietary fat intake and the risk of coronary heart disease in women. N Engl J Med 1997;337:1491-1499. 4. Ascherio A, Rimm EB, Giovannucci EL, Spiegelman D, Stampfer M, Willett WC. Dietary fat and risk of coronary heart disease in men: Cohort follow up study in the United States. BMJ 1996;313:84-90. 5. Esrey KL, Joseph L, Grover SA. Relationship between dietary intake and coronary heart disease mortality: Lipid research clinics prevalence follow-up study. J Clin Epidemiol 1996;49:211-216. 6. Pietinen P, Ascherio A, Korhonen P, et al. Intake of fatty acids and risk of coronary heart disease in a cohort of Finnish men – The alpha-tocopherol, beta-carotene cancer prevention study. Am J Epidemiol 1997;145:876-887. 7. Hu FB, Stampfer MJ, Rimm EB, et al. A prospective study of egg consumption and risk of cardiovascular disease in men and women. JAMA 1999;281:1387-1394. |
Casein Diet Lowers Lipoprotein(a) Levels
Recently, Lp(a) has received much attention for its possible role in CHD. This new risk factor was initially thought to be unaffected by diet, however, a recent study by Nilausen and Meinertz shows that dietary casein can dramatically lower plasma Lp(a) concentrations. The casein protein diet decreased Lp(a) levels much more than a soy protein rich diet; however as predicted, the soy diet was more effective in lowering total and LDL cholesterol levels.
Nine healthy normolipidemic males between 21 and 64 years of age with a BMI of 21.7 to 25.1 kg/m2 consumed 3 different diets. The diets were: a self-selected baseline diet, a liquid soy diet containing 20% of calories as soy protein, and a liquid casein diet with 20% of calories as casein. Subjects consumed each diet for 33-45 days with a washout period in-between. The test diets consisted of 20% of calories from protein as calcium caseinate or soy protein isolate, 55% CHO from cornstarch hydrolysate, and 25% fat high oleate safflower oil. Cholesterol was added to the soy protein diet to equal the casein diet’s level of 55 mg/MJ and the calcium level in the soy diet was adjusted to equal the casein diet.
Compared with the self-selected diet, both test diets decreased plasma lipid and lipoprotein levels. Total cholesterol levels decreased by 42 mg/dl and 40 mg/dl with the soy protein and casein diets, respectively. The LDL cholesterol, HDL cholesterol, and TAG levels decreased by 34 and 23 mg/dl, 7 and 12 mg/dl, and 8 and 15 mg/dl, respectively with the soy and casein diets. Only the plasma HDL cholesterol concentrations were significantly different between the 2 protein diets. However, plasma Lp(a) concentrations following initiation of the casein diet were almost 2 times lower than during intake of the soy diet or the self-selected diets. The average Lp(a) levels following the self-selected, soy protein, and casein diets were 92.1, 93.5, and 44.7 mg/dl, respectively. However, there was a wide individual variation in Lp(a) levels and the magnitude of change was directly correlated to baseline Lp(a) during the self selected diet phase. During the soy diet period, subjects’ Lp(a) levels slightly increased before falling to the baseline level, while the Lp(a) levels steadily decreased during intake of the casein diet to 65% below baseline.This study showed that a liquid casein diet was effective in lowering plasma Lp(a) levels compared to a soy protein diet in healthy men. But in spite of the lower Lp(a), it is too early to assume that this diet is an antiatherogenic diet leading to reduced CHD. For example, this diet consisted of 20% casein, which is difficult for an average American to tolerate. Also, at this point the researchers do not know what mechanisms are involved in the observations or if it’s actually casein protein rather than what’s missing in the soy protein and self selected diet that might cause elevated Lp(a) levels.
Nilausen, K, Meinertz, H. Lipoprotein (a) and dietary proteins: casein lowers lipoprotein(a) concentrations as compared with soy protein. Am J Clin Nutr. 1999;69:419-425.
Minority Population and CVD Risks
In this diverse country, people of different ethnic origins are battling CVD risks with very different results National Health and Nutrition Examination Survey (NHANES III, 1988-1994), minority children h. For example, based on the third National Health and Nutrition Examination Survey (NHANES III, 1988-1994), minority children have a higher number of risk factors for CVD than white children. Also, even between minority groups, there are major differences in their risk for CHD.
Using NHANES III data, Winkleby et al. reported that black and Mexican-American children had more CVD risk factors than whites even after socioeconomic status was adjusted in the analysis. Based on questionnaires and medical examination data of 2,063 white, 2,769 black, and 2,854 Mexican-American children, investigators found that a higher percentage of minority children lived below the poverty level, had parents with less formal education, and exhibited a greater number of CVD risk factors than their white counterparts. Also, compared to white children, minority children had more CVD risk factors and negative life style factors at an earlier age. For example, young minority girls between 6-9 years old had a higher BMI (17.7 kg/m2) and consumed more calories from fat (35.1%) than white girls of the same age, 17.1 kg/m2 and 33.3%, respectively. This trend continued in older minority girls between 18-24 years old with an average BMI of 25.5 compared to 23.1 in white girls. Black children had higher blood pressure and hemoglobin A1c levels than white or Mexican-American children. However, among boys, black boys ate a higher percentage of calories from fat than both Mexican-American and white boys and the hemoglobin A1c levels were higher for minority boys than white boys. On the other hand, white children of all ages smoked more than minority children. This was especially true in white children from lower educational homes.
This national, cross-sectional survey indicates that minority children are at a high risk of future CVD and interventions are warranted even in these young children to counter this negative trend. Current data suggest that heart health programs should begin to target children as young as 6-9 years old and to custom tailor programs for different ethnic groups for maximum benefit. Sundquist et al. also reported differences in CVD risk among subgroups of Mexican-American groups. Based on the NHANES III data, among Mexican-Americans, US born, Spanish-speaking Mexican-Americans had the highest risk of CVD followed by US born, English-speaking Mexican-Americans and the lowest risk in Mexico born Mexican-Americans. The age and education level adjusted 10 year CHD mortality rates for US born, Spanish-speaking Mexican men and women were 27.5 and 11.4, respectively, per 1,000 persons. The 10-year mortality rates were 22.5 and 7.0 per 1,000 persons in the highly assimilated English-speaking Mexican-American men and women, and 20.0 and 6.6 in the first generation Mexican-Americans. Also, Spanish-speaking Mexican-Americans had the highest levels of primary CVD risk factors while Mexico born Mexican-Americans had the least CVD risk factors. The levels of CVD risk factors for US born, English-speaking Mexican-Americans were very similar to non-Hispanic whites in the general population. Compared to first generation Mexican-Americans, all US-born Mexican-Americans smoked more and had higher BMI levels. However, when CVD risk factors were analyzed based on education level, English-speaking and Spanish-speaking Mexican-American men in the highest education group had the same risk factors for CVD.
Current findings from 2,791 Mexican-Americans, aged 25 to 64 years, in the NHANES III confirmed the researchers initial hypotheses that less assimilated Spanish-speaking Mexican-Americans would have the highest CHD risk since “they may have lost some of the advantages associated with the Mexican lifestyle without gaining the advantages associated with acculturation into the English-speaking culture.” This heterogeneity in CVD risk factors among Mexican-Americans indicated that certain sub-populations need more intensive intervention programs to lower their CVD risk profile.
Sundquist, J. Winkleby, M.A. et al. Cardiovascular risk factors in Mexican American Adults: A transcultural analysis of NHANES III, 1988-1994. Am J Public Health. 1999;89:723-730.
Winkleby MA, Robinson TN, Sunquist J, et al. Ethnic variation in cardiovascular disease risk factors among children and young adults. Findings from the third national health and nutrition examination survey, 1988-1994. JAMA. 1999;281:1006-1013.
Aging and CHD Risk Factors in Women
For a long time, the American public viewed CHD as primarily a disease which afflicted males, but thanks to better media coverage, women are starting to realize that heart disease is also a leading cause of death in their gender. This message is especially important since CHD risk factors increase dramatically with age in women. A Finnish study by Jousilahti et al. specifically addresses the effects of gender difference in CVD risk factors in 14,786 adults between 25-64 years old. The 7,090 men and 7,696 women in the study were initially recruited in either 1982 and 1987 and followed through 1994. During this time, 520 CHD incidences and 231 CHD death were reported in males compared with 209 CHD incidences and 63 CHD death in females. As a collective group, males had higher plasma total cholesterol, blood pressure, and BMI; lower plasma HDL cholesterol levels; and more smoked and had diabetes relative to the female subjects. Similar risk factors were noted in the 24-49 age group, however, women in the 2 older groups had similar or higher plasma total cholesterol levels, blood pressure, and BMI than their male counterparts. The plasma HDL cholesterol was still higher in females than males but lower than in the youngest female group. The percentage with diabetes increased with age, but at a similar rate between the sexes. In univariate analysis, male gender was associated with a RR of 3.38 for CHD incidence and 5.00 for mortality but decreased to 2.31 and 3.20 for incidence and mortality, respectively, based on multivariate analysis using other major CHD risk factors. The HDL/total cholesterol ratio and smoking were 2 leading determinants of the sex difference in CHD risk.
This investigation found that younger women had lower levels of CHD risk factors compared to men of the same age, but this was not found in older females. Plasma total cholesterol, systolic blood pressure, BMI, and HDL/total cholesterol ratio in older females were all indicative of a more atherogenic profile than older males exhibited, indicating that the risk of CHD increases rapidly in females as they age. This study poses the challenging public health task of lowering CHD risk among middle-aged men while preventing the marked increase in CHD risk with aging in women.
Jousilahti P, Vartiainen E, Tuomilehto J. et al. Sex, age, cardiovascular risk factors, and coronary heart disease. A prospective follow-up of 14,786 middle-aged men and women in Finland. Circulation. 1999;99:1165-1172.
Stanol-Containing Margarines Lower Plasma Cholesterol Levels
Besides the traditional dietary and pharmacological methods to lower an elevated plasma cholesterol, for the past several years a stanol-ester containing margarine has been available in Finland. Now, a new study by Hallikainen and Uusitupa shows it is also possible to significantly reduce total cholesterol and LDL cholesterol levels using a low-fat stanol ester-containing margarine in a low-fat, low-cholesterol diet. Consumption of the wood stanol ester-containing margarine (WSEM) lead to a 47 mg/dl (18.3%) decrease in plasma total cholesterol levels in 18 subjects on the WSEM diet. Decreases of 38 mg/dl (15.7%) and 19 mg/dl (7.7%) in total cholesterol were observed in 20 subjects consuming the vegetable oil stanol ester-containing margarine (VOSEM) and in 17 adults on the control diet. The plasma LDL cholesterol levels decreased by 41 mg/dl (23.6%), 31 mg/dl (18.4%), and 17 mg/dl (9.9%) following 8 weeks of the WSEM, VOSEM, and control diets, respectively. Although the absolute change in total and LDL cholesterol levels were greater with the WSEM diet than with the VOSEM diet, the values were not significantly different. The effects of dietary stanol-esters on plasma HDL, TAG, retinol, beta-carotene, and alpha-tocopherol were not significant.
The fifty-five subjects in this 12-week double-blind trial were randomly assigned to one of the 3 low-fat margarine diets following a 4-week baseline diet. The control diet consisted of 28-30% of calories from fat, 20% protein, 50-52% CHO, 23.8 mg/MJ cholesterol, and 25 grams low-fat margarine/d. In addition to these nutrients, the WSEM diet contained 2.31 gm sitostanol and 0.19 gm campestanol, while the VOSEM diet contained 2.16 gm sitostanol and 0.69 gm campestanol. Unlike sitostanol’s proven ability to inhibit cholesterol absorption, the effects of campestanol in inhibiting cholesterol absorption have not yet been firmly confirmed.
These results from this study indicate that low-fat plant stanol ester-containing margarines are more effective in reducing plasma cholesterol levels of hypercholesterolemic adults than a low-fat, low-cholesterol diet alone. The levels achieved were similar to outcomes following initiation of some cholesterol lowering drugs. The sitostanol and campesterol in the margarine decrease plasma total and LDL cholesterol levels without adversely affecting HDL and TAG levels, by competing with both dietary and biliary cholesterol absorption in the small intestine. Finally, the compliance rate on the diets was high indicating that subjects tolerated the experimental diets well.
Hallikainen MA, Uusitupa MI. Effects of 2 low-fat stanol ester-containing margarines on serum cholesterol concentrations as part of a low-fat diet in hypercholesterolemic subjects. Am J Clin Nutr. 1999;69:403-410.
Very Low-Fat Diet Associated with Small LDL
Contrary to a common belief, a very low-fat diet might be associated with a negative plasma lipoprotein profile. As reported in 1994 and 1995, the current study by Dreon et al. found that a low-fat, high CHO diet resulted in some males with an LDL subclass phenotype A to convert to the more atherogenic phenotype B. Instead of having large buoyant LDL associated with phenotype A, following a 10% fat and 76% CHO diet for 10 days resulted in 32% of the study subjects to convert to a phenotype B profile with small dense LDL particles.
Thirty-six participants in the study were specifically recruited from 2 earlier studies based on the finding that their phenotype A status did not change following initiation of a 20-24% fat diet. This randomized, cross-over study allowed the researchers to test the effects of a very low-fat diet, 10%, on plasma lipid and lipoprotein concentrations. All subjects consumed both the usual diet with 32% of calories from fat (10.8% SFA, 11.8% MUFA, 6.9% PUFA, 52% CHO, 14% protein, and 295 mg cholesterol) and the very low-fat diet of 10.4% calories from fat (2.7% SFA, 3.7% MUFA, 2.6% PUFA, 76% CHO, 15% protein, and 301 mg cholesterol) for 10 days each. Following each diet, plasma lipids, lipoproteins, and lipoprotein subclasses were analyzed. Total calories were regularly adjusted to maintain stable weight.
As in the previous studies, the very low-fat diet resulted in increased plasma TAG levels, VLDL subfractions mass, smaller LDL particles (LDL III and LDL IV), and apo B concentrations. In contrast, the masses of small IDL, LDL cholesterol, mass of large LDL I, HDL cholesterol, mass of HDL2 and HDL3, and apo A levels in plasma decreased. With the very low-fat diet, 12 men converted to phenotype B. The difference in lipoprotein parameters between stable phenotype A subjects versus new phenotype B subjects during the usual diet was not significantly different; however, the plasma lipoprotein profile was much more atherogenic in the second group with intake of a 10% fat diet. The concentration of plasma TAG and smaller LDL III and LDL IV subfractions were higher, while LDL I and HDL cholesterol levels were lower. The LDL cholesterol level was not significantly different in either group. The comparison of plasma lipid and lipoprotein concentrations during the 10% fat diet with the 20-24% fat diet showed that the lower fat diet resulted in higher plasma concentrations of VLDL, apo B, and HDL3. Also, rather than decreasing plasma LDL cholesterol levels compared to the 20-24% fat diet, the very low-fat diet increased plasma LDL by 27 mg/dl in new phenotype B men. There was no change in plasma LDL cholesterol level between the very low-fat diet and the 20-24% diet in the stable phenotype A group.
At this point researchers can not explain the mechanisms involved or the dietary factors responsible, high CHO versus very low-fat, for the changes in LDL phenotype in a third of study cohort. However, they suspect genetics is a key factor in this outcome. Finally, these data raise serious issues regarding the advisability of a very low-fat diet to lower the CHD risk as this diet can result in a negative plasma lipid profile in some individuals.
Dreon, DM, Fernstrom, HA, Williams, PT. A very-low-fat diet is not associated with improved lipoprotein profiles in men with a predominance of large, low-density lipoproteins. Am J Clin Nutr. 1999;69:411-418.
Long-term Exercise Associated with Improved Immunological Markers of CVD
Beneficial effects of exercise against CVD have been firmly established, however, the mechanism behind this protection is unclear. According to Smith et al., one possible solution to this multi-factorial question lies in one’s immune system. By measuring changes in atherogenic and atheroprotective cytokine levels following a 6-month exercise program in 43 adults (18 men and 25 women) the investigators observed a beneficial effects of exercise on blood mononuclear cell production of cytokines. The average duration and frequency of supervised exercise was 70 minutes for twice a week of aerobic exercises and weight lifting.
The atherogenic cytokines, interferon gamma (IFN-gamma), tumor necrosis factor (TNF-alpha), and interleukin (IL) 1-a levels produced by blood mononuclear cells fell by 58.3% and atheroprotective cytokines, IL-4, IL-10, and transforming growth factor beta (TGF-ß) levels increased 35.9% following the exercise period. The C-reactive protein levels which represent CHD risk, also decreased from baseline. The changes in both atherogenic and atheroprotective cytokine levels were directly correlated with duration of walking, running, cycling, rowing, climbing, skiing, and an aerobic program.
IFN-gamma and TNF-alpha cytokines are found in atherosclerotic lesions and thought to be involved in atherogenesis. The decrease in IFN-gamma and TNF-alpha and increase in TGF-ß and IL-10 production after a long-term exercise program suggests protection against ischemic heart disease. These data show that besides weight loss and improved lipoprotein levels, exercise can decrease CHD risk by improving the blood cytokine profile.
Smith JK, Dyes R, Douglas JE, et al. Long-term exercise and atherogenic activity of blood mononuclear cells in persons at risk of developing ischemic heart disease. JAMA. 1999;281:1722-1727.
Mediterranean Diet Reduces Secondary Cardiac Events
Results from to the Lyon Heart Study indicated that subjects with prior MI who consumed a Mediterranean type diet were less likely to experience secondary cardiovascular complications during the 46 month follow-up compared with controls on a prudent Western diet. Only 14 of 218 subjects on the Mediterranean diet suffered nonfatal MI or cardiac death compared with 44 of 204 controls. The incidence of both major and minor secondary cardiac events were 81 in the experimental group and 136 in the control group. Based on the dietary records from a subset group, the control group consumed higher amounts of total fat, saturated fat, and cholesterol, while experimental subjects had higher intakes of linolenic acid and dietary fiber; alcohol intake was the same for the 2 groups. Other cardiac risk related parameters, such as plasma lipid and lipoprotein concentrations, blood pressure, and BMI were similar in the control and experimental groups. However, when other CVD risk factors were included in the analysis, the data showed that “a low-fat Mediterranean diet does not quantitatively alter the usual relationship between the risk factors and recurrence rate.” The conditional risk ratios for diet was 0.28 compared with age (0.99), smoking (1.65), total cholesterol (1.28), systolic blood pressure (1.02), leukocyte count (2.84), and aspirin (0.59) for the primary outcomes of CVD death and nonfatal MI. These data indicate that smoking, total cholesterol, and leukocyte counts have a stronger impact on CHD risk than diet.
This study confirms the findings from an earlier intermediate analysis from the same cohorts at 27 months. The Mediterranean diet, high in fruits, vegetables, fish, and olive oil, was associated with a lower risk of CHD recurrence. The positive outcome obtained following the Mediterranean diet with high linolenic acid was independent of other major CHD risk factors on the recurrence rate.
de Lorgeril, M, Salen P, Martin, J et al. Mediterranean diet, traditional risk factors, and the rate of cardiovascular complications after myocardial infarction. Final report of the Lyon Heart Study. Circulation. 1999;99:779-785.
|
Editor’s Comment Findings from the Lyon Heart Study clearly show that there is more to managing CHD than simply reducing plasma cholesterol levels. Even with similar end lipid and lipoprotein levels, the rate of cardiac death and nonfatal infarction in the experimental group was 1.24 per hundred patients per year compared with 4.07 per hundred patients per year in the control group. Thus suggesting that the difference in nutrients, especially linolenic acid, in the experimental diet might have had a protective effect on CHD risk in the study cohorts. |
Editorial: I Know What I Know. Don’t Confuse Me With Facts
It’s usually hard for most of us to say “I was wrong.” But it seems to be almost impossible for the exin Nutrition Close-Up over the past half dozen years there are many reperts who propose dietary recommendations. As documented in Nutrition Close-Up over the past half dozen years there are many reported epidemiological studies showing a null relationship between dietary cholesterol, plasma cholesterol, and CVD incidence. Clinical studies and meta-analyses also demonstrate that dietary cholesterol has little effect on plasma cholesterol levels in most individuals. Even though the evidence shows that dietary cholesterol isn’t really related to either high plasma cholesterol or heart disease risk, consumers are still told that getting the dietary cholesterol out is a big step towards a heart healthy diet. And it would seem that, based on the responses to the Harvard School of Public Health JAMA report on eggs and heart disease, few in the dietary recommendations arena are willing to even consider informing the public that the changes they’re making are of little value.
This large prospective study of egg consumption and CVD risk in men and women was tagged as “just a single report,” albeit in over 117,000 people followed for 8 to 14 years. Unfortunately, those in health promotion seem unable to expand their perceptions to include these findings with a long list of studies coming to the same conclusion: eggs are not the CVD risk so many religiously believe. And some of the other comments in response to this report were equally short-sighted.
“Egg consumption is associated with eating foods high in saturated fat such as bacon, red meat and whole milk.””most people eat two eggs, rather than one egg in a serving— a single meal that contains double the amount of suggested (daily) dietary cholesterol.’’ “most of the study participants were health professionals who ate well anyway and tended to eat fewer eggs.””eggs can raise cholesterol significantly in someone who already eats a lot of other animal fats.””The American Heart Association and other responsible public health associations won’t change their guidelines of 3-4 eggs per week.”
Clearly many of the responses were not well rationalized. Based on this logic we should ban broccoli because of all the cheese sauce used! Do we really believe that if people who do eat high saturated fat foods would only not eat eggs they’ll get rid of those items, or that if people who avoid high saturated fat foods eat eggs their prudent diet will be subverted? And what is lost in the comment about two egg servings is that the 300 mg cholesterol per day recommendation is an average over days or a week. Whether I choose to eat 7 eggs a week one a day or a couple every few days really shouldn’t matter [unless I want to market those daily cholesterol calculators]. And the argument that these were somehow unique populations fails to recognize that what the study shows is that eggs are clearly not a problem in a healthy diet, it’s the saturated fat, excess calories, obesity, lack of physical activity, etc., etc., etc. And how does one conclude that 18,900 people eating 5 or more whole eggs per week is a low egg consumption when the average total egg consumption in the USA is 4.5 eggs per week? The comment regarding “other animal fat” shows an ignorance of the evidence that plasma cholesterol responses to dietary cholesterol in humans is independent of dietary fat type or amount. The combined result of all these expert opinions was nothing more than to further confuse the issue for consumers while not admitting that maybe a 25 year old opinion could maybe be wrong.
Amazingly, some dismissed the findings of this report on the day of its publication with the “expert opinion” that the results had no bearing on nutritional recommendations and policies. No evaluation, no deliberation, no discussion, no incorporation of the data into the existing body of knowledge; only summary dismissal of findings which disagree with opinions. This doesn’t seem to be a rationale formulation of public nutrition policy, or evidence of scientific evaluation of new research findings. It would seem that once nutritional policies are set and solidified, there are no adjustments or corrections based on science? This would seem to be a case of guilty until proven innocent, with the complication that there never ever seems to be enough proof.
Most countries do not bother having a dietary cholesterol, much less egg, restriction in their dietary guidelines. In 1972 it might have seemed like a good idea given the available evidence but after twenty-seven years of research results to the contrary maybe it’s time to reconsider this outdated and obsolete view that eggs are a health risk for the population. Egg consumption certainly isn’t a risk in countries with low rates of heart disease [Japan, 6.5 eggs per week; Spain, 5.1 eggs per week; and France, 5.0 eggs per week]. But then any changes in policy would require the ability to say “we were wrong.”
Donald J. McNamara, Ph.D.
Executive Editor, Nutrition Close-Up
 Executive Editor: Donald J. McNamara, Ph.D.
Executive Editor: Donald J. McNamara, Ph.D.
Writer/Editor: Linda Min, M.S., R.D.
Nutrition Close-Up is published quarterly by the Egg Nutrition Center. Nutrition Close-Up presents up-to-date reviews, summaries and commentaries on the latest research investigating the role of nutrition in health promotion and disease prevention, and the contributions of eggs to a nutritious and healthful diet. Nutrition and health care professionals can receive a FREE subscription for the newsletter by contacting the ENC.
![]()
